“More than 100 million U.S. adults are now living with diabetes or prediabetes, according to a new report released today by the Centers for Disease Control and Prevention (CDC). The report finds that as of 2015, 30.3 million Americans – 9.4 percent of the U.S. population –have diabetes. Another 84.1 million have prediabetes, a condition that if not treated, often leads to type 2 diabetes within five years.”
Diabetic Eye Exam and Diabetic Retinopathy
Diabetes is a metabolic disease in which the body’s ability to produce or respond to the hormone insulin is impaired. Not being able to produce insulin or use it effectively, leads to increase glucose levels in the blood. High levels of glucose circulating in the body become toxic to certain cells and specifically toxic to the pericytes, which are indispensable for proper equilibrium and to maintain normal blood vessel physiology. When those cells die, the blood vessels become leaky triggering a cascade of events that affect nearly every tissue and organ in the body.
Uncontrolled blood glucose levels can result in various eye conditions such as diabetic retinopathy, glaucoma, cataracts, and diabetic macular edema
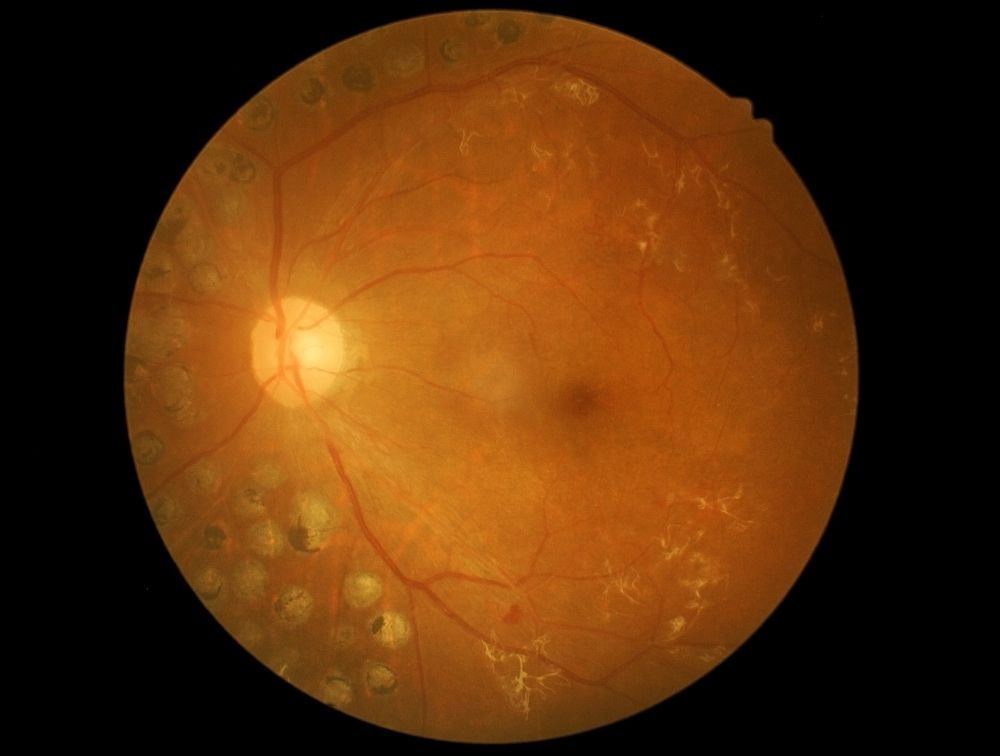
Diabetic retinopathy is an eye condition that occurs in people who have either Type 1 or Type 2 diabetes. Consistent high blood sugar from diabetes compromises the integrity of the tiny vessel walls in the retina, altering their structure and function. These fragile vessels may thicken, bleed, develop clots, develop balloon-like causing retinal tissue to swell and damage the cells in the retina.
In the early stages of diabetic retinopathy, they are usually no warning signs. The disease often progresses unnoticed until it affects vision. Bleeding from abnormal retinal blood vessels can cause the appearance of “floating” spots. These spots sometimes clear on their own. So the vision is not affected.
In most advanced stages, new abnormal blood vessels proliferate (increase in number) on the surface of the retina; fluid accumulation in the central part of the eyes. This will result in changes, loss of central vision, which can lead to scarring and separation of the retina from the back of the eye (retinal detachment) in the retina increasing the risk of permanent vision loss.
Diagnostic
Diabetic eye disease can be effectively detected through a comprehensive diabetic eye exam which includes different testing procedures. Our Dr in Long Island City would take a careful medical history. We need to know the nature of your diabetes (Type 1 or type 2), the duration of the disease, your fasting blood glucose level for that day as well as your hemoglobin A1C, which indicates your average blood glucose for the 3 months prior.
An exam is then performed with a careful dilated eye examination looking for any signs of diabetic retinopathy. We will send a report of findings to your primary care physician. If no signs of diabetic retinopathy are detected, the diabetic eye exam should be repeated yearly.
If the level of diabetic retinopathy warrants it, you will be referred to a retinal specialist for treatment.
Treatment for Diabetic Retinopathy
Treatment is based on the severity of the disease. Unfortunately, there are no non-invasive treatments.
Early Diabetic Retinopathy
Early or moderate non-proliferative diabetic retinopathy may not need treatment right away and an accurate blood sugar control can slow the progression of the disease.
Advance diabetic Retinopathy
In more advanced cases Proliferative diabetic Retinopathy or swollen the central area of the retina (macular edema) may require laser treatment or surgery.
Even after treatment for diabetic Retinopathy, your Doctor may require to follow up appointments to make sure the treatment was effective. Our doctor works with the most experienced Ophthalmologist (Retinal Specialist) to refer patients out when it is necessary and ensure you receive the utmost care in the area. Call us today for more information regarding our services.
To learn about about Diabetic Retinopathy:
Video of diabetic retinopathy
https://nei.nih.gov/health/diabetic/retinopathyi